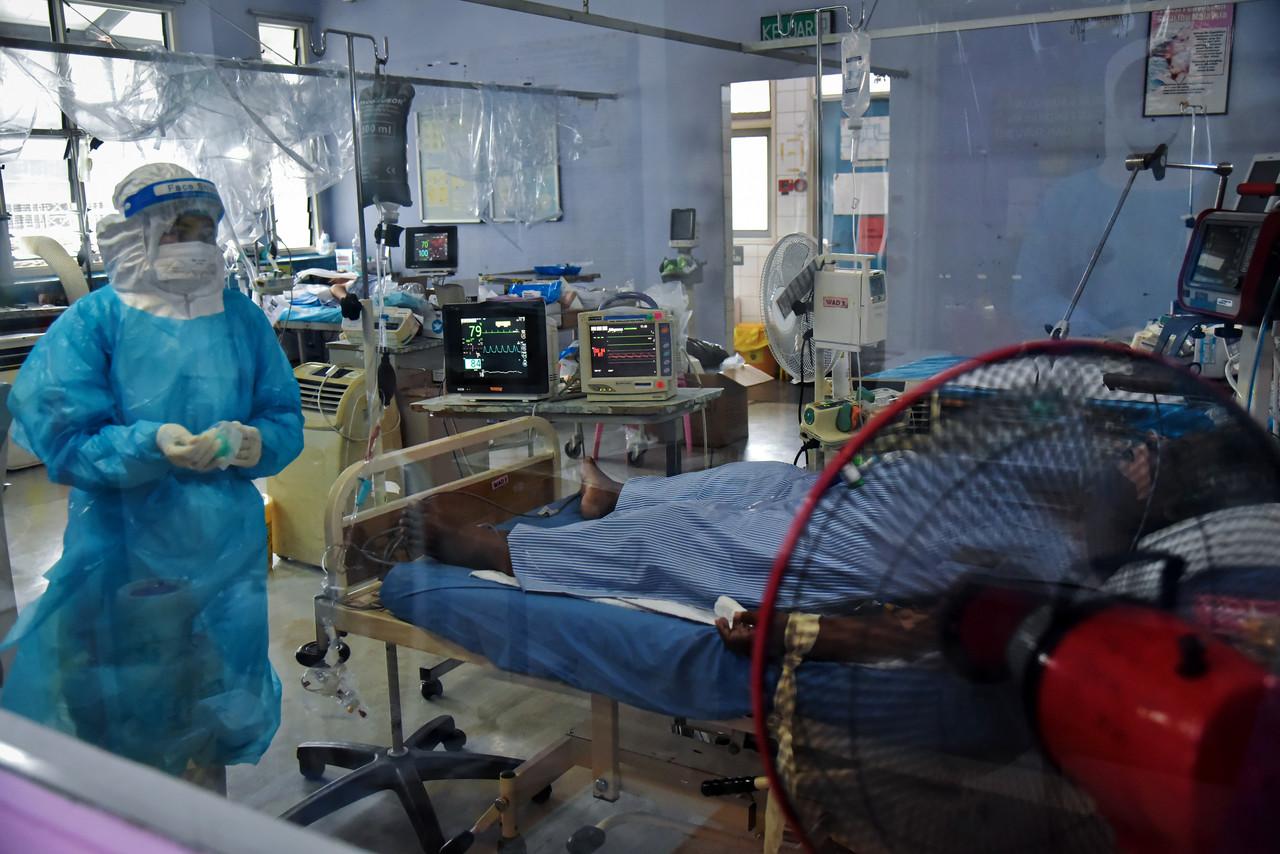
More focus on healthcare system, experts suggest on Covid-19 exit plan
They recommend using more related indicators to decide on transition from one phase to the next.
Just In
Public health experts have urged the government to consider more details especially regarding the state of the public healthcare system when deciding whether to move from one phase of the National Recovery Plan for Covid-19 to the next.
The three key indicators currently in use are the daily caseload, hospital capacity and vaccination rate.
Dr Malina Osman, an epidemiologist from Universiti Putra Malaysia, suggested that the government also take into consideration the number of active cases and those brought in dead.
“It should be more specific, to look at the actual burden on our healthcare system.
“The number of new cases alone may not be adequate,” she told MalaysiaNow.
She suggested that the indicators be revised to this effect, to include among others the mortality rate and the number of Covid-19 patients who are in critical condition which she said should decrease to two-digit figures before the movement control order (MCO) is eased.
“It should be more specific, to look at the actual burden on our healthcare system.”
Once the healthcare system is able to operate normally without needing to focus primarily on Covid-19 patients, she said, restrictions could be relaxed.
“(What this means) is that our healthcare system will be able to offer other ordinary services which are now postponed due to the overwhelming numbers of Covid-19 patients,” she said.
“This includes elective surgeries, screening and testing for other diseases.”
The four-phase National Recovery Plan, which will see the country’s various sectors reopening in stages, was announced by Prime Minister Muhyiddin Yassin on June 15.
Transition to the second phase will be subject to the number of daily new infections dropping below 4,000, the easing of pressure on the public health system and the rate of fully vaccinated people hitting 10% of the population.
In order to progress to the third stage, daily cases must drop below 2,000 while 40% of the population must be fully vaccinated.
Transition to the final stage, meanwhile, will be contingent on daily infections falling below 500 and 60% of the population being fully vaccinated.
Dr Sanjay Rampal, an epidemiologist at Universiti Malaya, proposed the recalibration of MCO conditions based on sector, saying transmission effects vary from one to the next.
He said activities such as shopping, physical recreation and dining in open areas were less likely to affect disease transmission than working or studying in congested areas.
“We should use appropriate epidemiological indicators as thresholds for SOPs.
“Localising SOPs from a national level to region, state or district will improve the benefit-to-cost ratio,” he said, acknowledging however that this would complicate operations.
He also suggested that SOPs be revised using an algorithm that integrates factors such as total numbers and case density according to population size, percentage of community transmissions and transmissibility or Rt.
“It may take a very long time for cases to reach our dream numbers.”
Other possible indicators include the utilisation of preventive public health services by taking into account the length of time from testing to contact tracing as well as use of ICU wards, he said.
Dr Raj Kumar Maharajah, who heads the Medical Practitioners Coalition Association of Malaysia, said the government’s present indicators provided a solid base on which to plan its next moves.
But he suggested that the R-naught or infectivity rate be the main factor in deciding on the capacity of the healthcare system to handle Covid-19 cases.
“It should one of the main indicators to tell if our health system is reaching the brink of collapse and if it can cope any further,” he said.
“If all of these are in the tolerable range, then we are okay.”
He also expressed reservations about the goal of reaching 4,000 daily cases, saying it might not be achieved any time soon.
“It may take a very long time for cases to reach our dream numbers,” he said. “I think it will take a very long time for cases to go below 4,000.
“We are trapped between the devil and the deep blue sea,” he added. “If you don’t die of Covid, you will die of hunger, so we need to think carefully and balance things out properly.”
Subscribe to our newsletter
To be updated with all the latest news and analyses daily.